TMS Therapy for Depression & OCD
For Patients Who Have Not Improved with Medication
What is TMS?
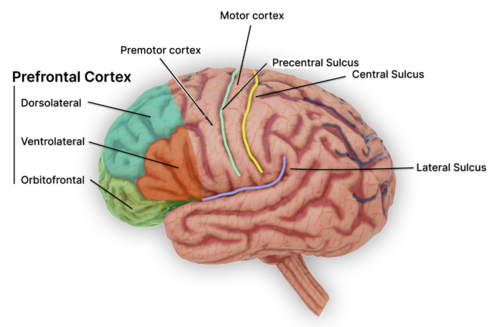
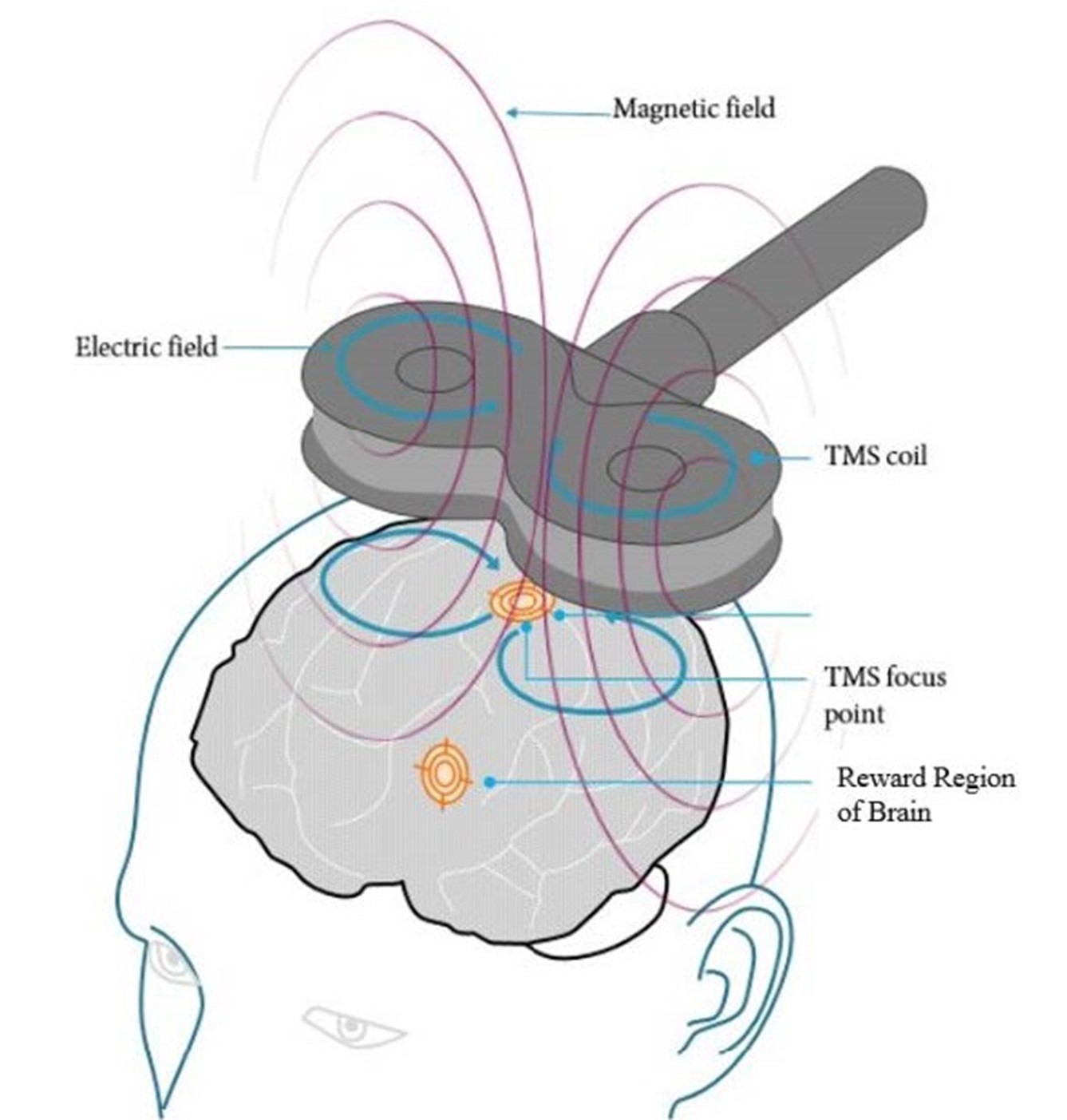
Transcranial Magnetic Stimulation (TMS) is an FDA-approved, non-medication treatment for depression and OCD. TMS uses gentle magnetic pulses to stimulate areas of the brain involved in mood regulation that may be underactive in depression. Over time, this stimulation helps restore normal brain activity and improve mood, energy, and motivation.
TMS is commonly used when medications have not helped enough or have caused difficult side effects.
Who is a Candidate for TMS?
TMS may be right for patients who:
- Have tried 2 or more medications without enough improvement
- Have medication side effects
- Have depression that keeps returning
- Are looking for a non-medication treatment
- Have OCD
TMS may not be appropriate for patients with:
- Certain metal implants in the head
- Some implanted medical devices
- Uncontrolled seizure disorders
What Treatment is Like
- Treatments last about 18–20 minutes
- Treatments are 5 days per week for 6–9 weeks
- You are awake and can talk during treatment
- You can drive yourself to and from treatment
- Most patients return to normal daily activities after each session
Our team monitors your progress throughout treatment and adjusts the treatment if needed.
- Video Goes Here -
Why Choose Our TMS Program
Choosing where to receive TMS treatment matters. Experience, physician involvement, and individualized treatment planning can make a significant difference in outcomes.
Does TMS Work? (Outcomes)
Transcranial Magnetic Stimulation is an evidence-based treatment for depression, particularly for patients who have not improved with medication.
National studies show:
- Approximately 50–60% of patients experience significant improvement
- Approximately 30–35% achieve remission
- Many patients experience relief that lasts months to over a year
Large real-world clinical registries using NeuroStar TMS show:
- About 69% of patients respond
- About 36% achieve remission
Outcomes are often higher in programs where a psychiatrist performs the consultation and mapping, treatment is individualized, and care is coordinated with the patient’s existing providers.
- Approximately 75-79% of our patients experience significant improvement
Approximately 50% achieve remission
TMS vs Antidepressant Medication
Antidepressant Medications
- Work throughout the entire body
- May cause side effects such as weight gain, fatigue, or sexual side effects
- The NIMH-funded, multi-year study, the STAR*D study involved around 4,041 patients. The remission rates with the first antidepressant trial were around 30% with trials two, three, and four; showing remission rates of around 13% by the fourth oral antidepressant trialed in a major depressive episode.
TMS Therapy
- Non-medication treatment
- Targets specific brain areas involved in mood regulation
- Minimal systemic side effects
- Patients remain awake and can drive themselves
- Remission rates are similar or better than additional medication trials in patients who have not responded to medications
TMS is often recommended for patients who have not improved with medications or cannot tolerate medication side effects.
Maintenance TMS - What Happens after the First 2 Months?
Depression can be a recurrent condition, which means symptoms may return over time. The goal of TMS is not only to improve symptoms, but also to help patients maintain that improvement.
After the initial course of TMS:
- Many patients remain well for months to over a year
- Some patients benefit from maintenance treatments
- If symptoms begin to return, booster treatments can be scheduled
We work with each patient to develop a long-term plan after TMS to help maintain progress and stability.
For Referring Providers
We value our relationships with psychiatrists, primary care providers, therapists, and other clinicians in the community and view TMS as a collaborative treatment.
When you refer a patient to our TMS program:
- The patient receives a comprehensive psychiatric evaluation
- All brain mappings are performed by a psychiatrist
- We provide updates on patient progress during treatment
- Medication management can remain with the referring provider, or we can assist if requested
- After completion of TMS, the patient is returned to the referring provider for ongoing care
- We remain available for maintenance TMS or future booster treatments if needed
Our goal is to support your patient’s recovery while maintaining your primary treatment relationship.
Am I a TMS Candidate? (Quiz)
Answer the following questions:
If you answered yes to most of these, you may be a candidate for TMS.
Insurance & Cost
- Most major insurance plans cover TMS
- We obtain prior authorization
- We review your benefits before treatment begins
- Financing options may be available
Contact Us
You do not have to continue feeling this way.
If you are not sure whether TMS is right for you, the first step is a consultation. We will review your history, prior treatments, and insurance coverage and help you determine if this is the right next step.
